What are the three types of skin problems?
Discover 'What are the three types of skin problems?' Uncover causes, symptoms, and treatments for these common dermatological issues.

What are the three types of skin problems?
Skin problems can vary widely, but there are three types that are particularly common and can cause distress for many individuals. These types of skin problems include acne, alopecia areata, and atopic dermatitis.
Key Takeaways:
- Acne, alopecia areata, and atopic dermatitis are three common types of skin problems.
- Acne occurs due to blocked skin follicles.
- Alopecia areata leads to hair loss in small, round patches.
- Atopic dermatitis is a skin disease that causes itching, redness, swelling, and other symptoms.
- These skin problems can cause distress for individuals and may require professional advice and treatment.

Understanding Acne
Acne is one of the most prevalent skin problems, affecting individuals of all ages, and can cause both physical and emotional discomfort. It is characterized by the appearance of pimples, blackheads, whiteheads, and sometimes even cysts on the skin. Acne occurs when the hair follicles become clogged with oil, dead skin cells, and bacteria.
Several factors contribute to the development of acne, including hormone fluctuations, excessive sebum production, genetics, and certain medications. It is important to note that acne can vary in severity, with some individuals experiencing mild breakouts while others may have more severe and persistent cases.
The Symptoms of Acne Include:
- Pimples, which can be red, inflamed, or contain pus
- Blackheads, characterized by small black or darkened bumps
- Whiteheads, which are small, flesh-colored bumps
- Cystic acne, which is deep, painful, and can leave scars
- Oily or greasy skin
While acne commonly affects the face, it can also appear on the back, chest, shoulders, and neck. Treatments for acne range from over-the-counter topical creams and gels to prescription medications, depending on the severity of the condition. Dermatologists may also recommend lifestyle modifications and skincare routines to manage and prevent future breakouts.

Alopecia Areata: Hair Loss in Patches
Alopecia areata is a dermatological condition characterized by sudden hair loss in round patches, which can be a source of significant concern for those affected. This condition occurs when the immune system mistakenly attacks the hair follicles, leading to hair loss. The exact cause of alopecia areata is unknown, but it is believed to be an autoimmune disorder.
Individuals with alopecia areata may experience hair loss on the scalp, eyebrows, eyelashes, and even other hair-bearing areas of the body. The patches of hair loss can vary in size and may progress over time. While the condition is not physically painful or contagious, it can have a profound impact on a person's self-esteem and emotional well-being.
Treatment options for alopecia areata vary depending on the severity and extent of hair loss. In some cases, hair may regrow spontaneously without treatment. However, individuals with more extensive hair loss or those seeking faster regrowth may consider options such as topical corticosteroids, injections of corticosteroids directly into the affected areas, or other immunosuppressive medications.
Key Points:
- Alopecia areata is an autoimmune condition that causes sudden hair loss in round patches.
- It can affect the scalp, eyebrows, eyelashes, and other hair-bearing areas of the body.
- Treatment options include topical corticosteroids, injections of corticosteroids, and immunosuppressive medications.
- Managing the emotional impact of hair loss is also an important aspect of alopecia areata treatment.
Individuals experiencing hair loss or noticing round patches of hair loss should consult a dermatologist for an accurate diagnosis and appropriate treatment options. While there is currently no cure for alopecia areata, there are ways to manage the condition and support hair regrowth.
Understanding Atopic Dermatitis
Atopic dermatitis, also known as eczema, is a chronic skin condition that can cause intense itching, inflammation, and discomfort. It is characterized by red, dry, and scaly patches on the skin, which can appear anywhere on the body. This condition is most commonly found in infants and young children, but it can also persist into adulthood.
There are several factors that contribute to the development of atopic dermatitis. It is believed to have a genetic component, as individuals with a family history of allergies or asthma are more likely to develop this skin condition. Environmental factors, such as exposure to certain allergens or irritants, can also trigger flare-ups. Additionally, a weakened immune system and an impaired skin barrier function play a role in the development of atopic dermatitis.
Treatment for atopic dermatitis aims to alleviate symptoms, reduce inflammation, and prevent flare-ups. This may involve the use of topical corticosteroids or other prescription medications to manage itching and inflammation. Moisturizers and emollients help to hydrate the skin and restore its natural barrier function. In some cases, phototherapy or systemic medications may be recommended.
Individuals with atopic dermatitis can also take steps to manage their condition and prevent flare-ups. This includes avoiding known triggers, such as certain soaps, detergents, and fabrics that can irritate the skin. Maintaining a regular skincare routine, including gentle cleansing and moisturizing, is essential. It is also important to keep the skin well-hydrated, avoid scratching, and manage stress levels, as stress can worsen symptoms.

Causes of Skin Problems
Skin problems can arise due to a combination of genetic, environmental, and lifestyle factors, making them a complex issue to address. Understanding the underlying causes is crucial in managing and preventing such dermatological conditions.
1. Genetic Predisposition: Some individuals may have a genetic predisposition to certain skin problems. Inherited genes can influence the skin's response to environmental factors and determine susceptibility to conditions like acne, alopecia areata, and atopic dermatitis.
2. Environmental Factors: External factors such as pollution, ultraviolet radiation, and exposure to harsh chemicals can contribute to skin problems. These environmental pollutants can disrupt the natural balance of the skin, leading to inflammation, allergic reactions, and other dermatological issues.
3. Lifestyle Choices: Unhealthy lifestyle choices, including poor diet, lack of exercise, smoking, and excessive alcohol consumption, can take a toll on the skin. These habits can compromise the skin's integrity, impair its ability to heal, and increase the risk of developing various skin problems.
Other Factors Contributing to Skin Problems:
- Hormonal Changes: Hormonal fluctuations, such as those occurring during puberty, pregnancy, and menopause, can trigger skin problems like acne and exacerbate other conditions.
- Stress: High levels of stress can disrupt the body's natural balance, leading to hormonal imbalances, impaired immune function, and increased inflammation, all of which can contribute to skin problems.
- Poor Skincare Routine: Inadequate skincare practices, such as the use of harsh products, failure to remove makeup properly, and lack of moisturization, can damage the skin's protective barrier and make it more susceptible to problems.
- Dietary Factors: Certain dietary choices, such as consuming excessive sugar, processed foods, and unhealthy fats, can promote inflammation and impact the health of the skin.
It's important to note that each individual may have unique factors contributing to their specific skin problem. Consulting a dermatologist or healthcare professional can provide personalized guidance on managing and treating these conditions effectively.
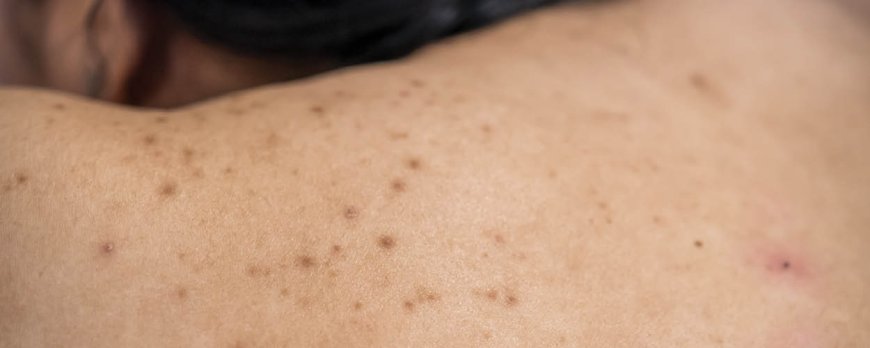
Symptoms of Skin Problems
Different types of skin problems may manifest with specific symptoms, which can range from mild to severe and may require medical attention. Recognizing these symptoms is crucial for timely intervention and effective treatment. Here are some common symptoms associated with various skin issues:
- Acne: The presence of blackheads, whiteheads, pimples, or cysts on the face, chest, back, or other areas of the body.
- Alopecia Areata: Hair loss in small, round patches on the scalp, eyebrows, eyelashes, or other hairy areas.
- Atopic Dermatitis: Intense itching, redness, dryness, and inflammation of the skin, often accompanied by oozing or crusting.
- Eczema: Red, itchy, and inflamed patches of skin, usually recurring or chronic in nature.
- Psoriasis: Thickened, scaly patches of skin, often silver or red in color, typically affecting the elbows, knees, scalp, or lower back.
- Rosacea: Persistent redness, visible blood vessels, and the presence of small bumps or pimples on the face.
- Seborrheic Dermatitis: Greasy, yellow or white scales on the scalp, face, or other areas, along with redness and itching.
It is important to note that these symptoms can vary in severity and presentation, depending on the individual and the specific skin problem. If you or someone you know is experiencing any of these symptoms or other concerning skin issues, it is advisable to seek professional advice for accurate diagnosis and tailored treatment. A dermatologist or healthcare professional can provide expert guidance and recommend appropriate interventions.
Treatment Options for Skin Problems
Treatment options for skin problems can vary depending on the specific condition, severity, and individual needs, with a range of approaches available to address these concerns. Here are some common treatments for acne, alopecia areata, and atopic dermatitis:
1. Acne:
- Topical treatments: Over-the-counter or prescription creams, gels, or lotions containing ingredients like benzoyl peroxide, salicylic acid, or retinoids can help unclog pores and reduce inflammation.
- Oral medications: In cases of moderate to severe acne, oral antibiotics or isotretinoin may be prescribed to control bacteria, inflammation, or oil production.
- Procedures: Dermatologists may recommend procedures such as chemical peels, microdermabrasion, or light therapy to treat acne and improve skin texture.
2. Alopecia Areata:
- Topical treatments: Corticosteroid creams or ointments can be applied to affected areas to reduce inflammation and promote hair regrowth.
- Injections: Corticosteroid injections directly into the bald patches can stimulate hair regrowth in some cases.
- Scalp irritants: Certain topical medications like anthralin or minoxidil may be used to irritate the scalp and encourage hair regrowth.
3. Atopic Dermatitis:
- Emollients and moisturizers: Regular use of fragrance-free moisturizers is essential to hydrate the skin and prevent dryness, itching, and flare-ups.
- Topical corticosteroids: Prescription-strength creams or ointments containing corticosteroids can help reduce inflammation and relieve itching.
- Immunomodulators: Non-steroidal creams like calcineurin inhibitors may be prescribed to manage flare-ups and reduce inflammation in sensitive areas.
- Phototherapy: Controlled exposure to ultraviolet light, either through natural sunlight or medical devices, can alleviate symptoms of atopic dermatitis.
It's important to note that these treatment options are general guidelines and may vary depending on individual circumstances. Consulting with a dermatologist or healthcare professional is crucial to receive an accurate diagnosis and personalized treatment plan for any skin problem.

Preventive Measures for Healthy Skin
Taking proactive steps to care for your skin can help prevent the occurrence of common skin problems and promote overall skin health. By adopting a consistent skincare routine and incorporating protective measures into your daily life, you can keep your skin looking its best and reduce the risk of developing skin concerns.
Here are some preventive measures to consider:
- Cleanse and moisturize: Start by cleansing your skin daily to remove impurities and excess oil. Follow up with a moisturizer to keep your skin hydrated and nourished.
- Protect from the sun: Apply a broad-spectrum sunscreen with an SPF of 30 or higher to shield your skin from harmful UV rays. Reapply every two hours, especially if you're spending time outdoors.
- Stay hydrated: Drink plenty of water to keep your skin hydrated from within. Proper hydration helps maintain the skin's natural moisture balance and supports a healthy complexion.
- Eat a balanced diet: Include fruits, vegetables, whole grains, and lean proteins in your diet. These nutrient-rich foods can provide essential vitamins and antioxidants that promote skin health.
Additionally, managing stress levels and getting enough quality sleep can contribute to healthy skin. Chronic stress can disrupt the skin's barrier function and trigger inflammation, while sufficient sleep allows the skin to repair and regenerate itself.
Remember, while these preventive measures can help maintain healthy skin, it's important to consult a dermatologist or healthcare professional if you experience any persistent skin concerns or have specific skincare needs. They can offer personalized advice and recommend suitable products or treatments tailored to your skin's unique requirements.
Seeking Professional Advice
If you are experiencing persistent or severe skin problems, it is advisable to seek guidance from a healthcare professional who specializes in dermatology. These professionals have the expertise and knowledge to accurately diagnose and treat a wide range of dermatological conditions, including acne, alopecia areata, and atopic dermatitis.
When you consult a dermatologist, they will thoroughly evaluate your skin concerns and medical history to determine the most appropriate course of action. They may recommend specific treatments, prescribe medication, or suggest lifestyle modifications to manage and improve your skin health.
Additionally, seeking professional advice can help prevent potential complications and ensure you receive personalized care. Dermatologists stay updated on the latest advancements in dermatology and have access to advanced diagnostic tools and treatment options.
Remember, each person's skin is unique, and what works for one individual may not work for another. By consulting a dermatologist, you can receive tailored advice and treatment plans that address your specific dermatological needs, increasing your chances of achieving healthier skin.
Lifestyle Factors and Skin Health
Lifestyle choices can significantly influence the health and appearance of your skin, and understanding their impact is crucial for maintaining skin health. Here are some key lifestyle factors that can affect your skin:
- Diet: A balanced diet rich in fruits, vegetables, and essential nutrients can promote healthy skin. On the other hand, consuming excessive sugar, processed foods, and unhealthy fats may contribute to skin issues.
- Stress: Chronic stress can trigger hormonal imbalances and inflammation, leading to various skin concerns like acne, eczema, and psoriasis. Incorporating stress management techniques such as exercise, meditation, and adequate sleep can help reduce the impact of stress on your skin.
- Sleep: Lack of sleep can disrupt the skin's natural repair process and weaken its ability to defend against environmental stressors. Aim for 7-9 hours of quality sleep each night to promote optimal skin health.
- Sun Exposure: Overexposure to the sun's harmful UV rays can cause premature aging, sunburn, and increase the risk of skin cancer. Protect your skin by wearing sunscreen, seeking shade, and wearing protective clothing.
It's important to note that everyone's skin is unique, and what works for one person may not work for another. If you have specific skin concerns or conditions, consulting with a dermatologist is recommended. They can provide personalized advice and recommend appropriate skincare products and treatments.
By making conscious choices to prioritize a healthy lifestyle, you can support your skin's natural functions and maintain its overall health and appearance.
Conclusion
Being aware of the three most common types of skin problems, including acne, alopecia areata, and atopic dermatitis, can empower individuals to seek appropriate care and take proactive steps towards achieving healthier skin.
Acne, characterized by blocked skin follicles, affects individuals of all ages and can be managed with various treatment options. Alopecia areata, which causes hair loss in small, round patches, can be distressing, but with early diagnosis and suitable treatment, individuals can regain their confidence. Atopic dermatitis, a skin disease that leads to itching, redness, and swelling, can be effectively managed with trigger avoidance and proper skincare routines.
By understanding the causes, symptoms, and available treatments for these dermatological conditions, individuals can make informed decisions about their skincare. It is also important to consider lifestyle factors, such as diet, stress, sleep, and sun exposure, which can impact overall skin health. Maintaining a consistent skincare routine and seeking professional advice when needed are crucial to maintaining healthy skin.
To promote skin health and prevent the development of skin problems, individuals should prioritize their well-being by adopting preventive measures, including regular cleansing, moisturizing, sun protection, and a balanced lifestyle. By taking these proactive steps and being aware of the various types of skin problems, individuals can improve their overall skin health and enhance their quality of life.
FAQ
What are the three types of skin problems?
The three types of skin problems are acne, alopecia areata, and atopic dermatitis.
What causes acne?
Acne is caused by blocked skin follicles.
What is alopecia areata?
Alopecia areata is a condition that causes hair loss in small, round patches.
What is atopic dermatitis?
Atopic dermatitis is a skin disease that causes itching, redness, swelling, and other symptoms.


































































































































