What does drug acne look like?
Discover the distinguishing features of drug acne. Understand 'What does drug acne look like?' with our concise and insightful guide.
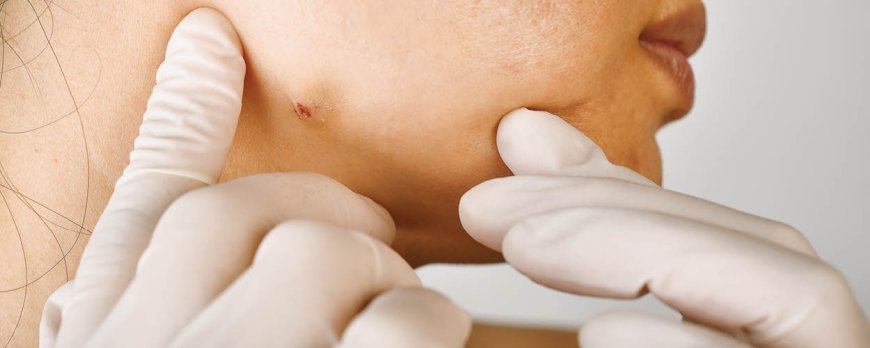
What Does Drug Acne Look Like?
Drug acne, also known as drug-induced acne or acneiform eruptions, is a common skin condition caused by certain drugs. It is characterized by a sudden eruption of inflammatory papules and pustules, often pruritic and follicular. Unlike typical acne, drug-induced acne does not have visible comedones preceding the skin lesions.
Various types of drugs can contribute to the development of drug acne. Systemic drugs such as corticosteroids, lithium, vitamin B12, thyroid hormones, halogen compounds, antibiotics, antituberculosis drugs, antiepileptic drugs, cyclosporin A, and isotretinoin have been linked to this condition. Additionally, topical products like cosmetics can also lead to acneiform eruptions, especially in women.
If you suspect you may have drug-induced acne, it is important to seek medical care to accurately identify and treat the condition. Discontinuing the use of the offending drug is often the first step towards remission of symptoms. Treatment options may include antihistamines to alleviate pruritus and oral antibiotics to address secondary infections.
Key Takeaways:
- Drug acne is caused by certain drugs and manifests as a sudden eruption of inflammatory papules and pustules.
- Visible comedones are typically absent in drug-induced acne.
- Systemic drugs and topical products can both contribute to the development of drug acne.
- Seeking medical care and discontinuing the use of the offending drug is crucial for accurate diagnosis and treatment.
- Treatment options may include antihistamines for pruritus and oral antibiotics for secondary infections.
Different Types of Drug Acne
Drug acne can manifest in different forms depending on the specific drug and individual characteristics. It is important to understand the various types of drug acne and the signs that indicate drug-induced skin eruptions. Here are some common types:
- Acne Vulgaris: This is the most common type of drug acne and is characterized by the presence of inflammatory papules, pustules, and comedones on the skin.
- Acneiform Eruptions: These eruptions resemble acne but are not true acne. They can be caused by systemic drugs or topical products, such as cosmetics.
- Drug-Induced Rosacea: Some medications can trigger a condition similar to rosacea, causing facial redness, flushing, and the appearance of small blood vessels on the skin.
- Perioral Dermatitis: This type of drug acne affects the area around the mouth and is characterized by small papules and pustules, often accompanied by redness and scaling.
To identify drug-induced acne, it is important to look for specific signs, such as the sudden onset of skin eruptions after starting a new medication or a change in dosage. It is advisable to consult a healthcare professional for a proper diagnosis and treatment.
Different Types of Drug Acne
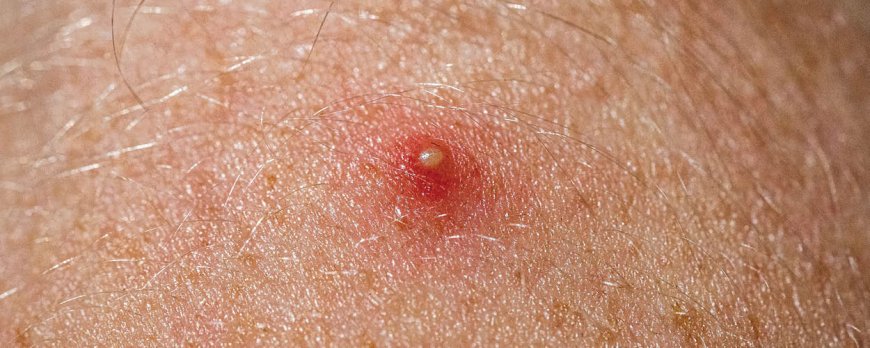
Characteristics of Drug Acne
Drug acne typically appears as a sudden eruption of inflammatory papules and pustules on the skin. These lesions are often red and swollen, and they may be accompanied by itching and a sensation of heat. Unlike traditional acne, drug-induced acne is not usually preceded by visible comedones, such as blackheads or whiteheads.
Identifying drug acne can be challenging, as it can resemble other skin conditions. However, there are some key characteristics that can help differentiate it from other types of acne. Firstly, drug-induced acne tends to develop rapidly after starting or altering medication. This sudden onset is often a clue that the acne is caused by a drug. Secondly, the distribution of the lesions may be different from regular acne. For example, drug acne may appear on areas of the body that are not typically prone to acne, such as the chest or back. Lastly, drug-induced acne may not respond to conventional acne treatments, which further supports its connection to medication use.
Common symptoms of drug-induced acne include:
- Inflammatory papules and pustules
- Redness and swelling
- Itching and discomfort
- Heat and tenderness
- Quick onset following medication use
- Unusual distribution of lesions
- Lack of response to traditional acne treatments
If you suspect that you may be experiencing drug-induced acne, it is important to consult a healthcare professional for an accurate diagnosis. They can review your medication history and help determine if there is a correlation between your acne and the drugs you are taking. In some cases, discontinuing the medication may lead to the resolution of symptoms. However, it is essential to follow your doctor's advice and not stop any medication without their guidance. They can also recommend appropriate treatment options to manage the acne and alleviate any discomfort you may be experiencing. Remember, seeking medical care is crucial for effective treatment and the overall health of your skin.
Systemic Drugs and Drug Acne
Certain systemic drugs, including corticosteroids, lithium, and antibiotics, can contribute to the occurrence of drug acne. These medications can disrupt the normal functioning of the skin and trigger the development of acneiform eruptions. Corticosteroids, commonly used to treat inflammatory conditions, can cause acne-like lesions due to their effects on the sebaceous glands. Lithium, a medication used to manage bipolar disorder, has been associated with the onset of acneiform eruptions.
Antibiotics, widely prescribed to treat bacterial infections, can also lead to drug-induced acne. These drugs can alter the composition of the skin's microbiome, promoting the growth of acne-causing bacteria. Additionally, other systemic drugs such as vitamin B12, thyroid hormones, halogen compounds, antituberculosis drugs, antiepileptic drugs, cyclosporin A, and isotretinoin have been linked to the development of drug acne.
It is important to note that not everyone who takes these medications will experience drug-induced acne. The occurrence of these acneiform eruptions can vary depending on individual factors such as skin type, genetics, and dosage of the drugs. If you are taking any of these systemic drugs and notice the onset of acne-like skin lesions, it is advisable to consult with a healthcare professional for diagnosis and appropriate management.
Identifying Drug Acne
- Sudden eruption of inflammatory papules and pustules
- Pruritic and follicular skin lesions
- Absence of visible comedones
Drug acne typically presents as a sudden outbreak of inflamed papules and pustules. These lesions may be accompanied by itchiness and affect the hair follicles. Unlike traditional acne, drug-induced acne does not usually involve the formation of blackheads or whiteheads. Knowing these characteristics can help in distinguishing drug acne from other types of acne and seeking appropriate treatment.

Topical Products and Drug Acne
In some cases, the use of certain topical products, particularly cosmetics, can lead to the formation of drug-related acne. These acneiform eruptions are characterized by the sudden appearance of inflammatory papules and pustules on the skin, which can be itchy and occur in hair follicles. Unlike traditional acne, drug-induced acne is not preceded by visible comedones.
When choosing cosmetics, it is important to consider the ingredients and their potential to cause acne. Some products may contain comedogenic ingredients that can clog pores and trigger an acne outbreak. These ingredients include oils, waxes, and certain synthetic compounds. Additionally, some individuals may have specific sensitivities or allergies to certain cosmetic ingredients, further exacerbating the risk of drug-induced acne.
To avoid or minimize the risk of drug acne caused by topical products, it is recommended to opt for non-comedogenic cosmetics. These products are specifically formulated to not clog pores and are less likely to trigger acne breakouts. It is also advisable to patch-test new cosmetics before applying them to a larger area of the face or body. This can help identify any potential adverse reactions before they lead to more widespread skin issues.
If you suspect that your acne is caused by a specific cosmetic product, discontinuing its use may lead to a resolution of the symptoms. However, it is always recommended to consult with a dermatologist or healthcare professional for a proper diagnosis and guidance on the most suitable treatment approach for drug-induced acne.
Treatment Options for Drug-Induced Acne
Treating drug-induced acne often involves medications like oral antibiotics to address secondary infections and antihistamines to alleviate pruritus. When it comes to managing the symptoms of drug-induced acne, a combination approach is typically employed to achieve optimal results.
Here are some treatment options commonly used for drug-induced acne:
- Oral antibiotics: In cases where drug-induced acne becomes infected, oral antibiotics may be prescribed. These medications help to eliminate the bacteria causing the infection and reduce inflammation within the skin.
- Antihistamines: Pruritus, or itching, is a common symptom of drug-induced acne. Antihistamines can help relieve this uncomfortable sensation and provide relief to the affected individuals.
- Topical treatments: Depending on the severity of the drug-induced acne, topical treatments such as retinoids or benzoyl peroxide may be recommended. These products work by reducing inflammation, unclogging pores, and promoting skin renewal.
- Discontinuation of the drug: In many cases, the most effective treatment for drug-induced acne is to stop taking the medication that is causing the skin eruption. Once the drug is discontinued, the symptoms of acne usually subside, and the skin can begin to heal.
It is important to note that treatment plans may vary depending on the individual and the specific medications involved. Consulting with a dermatologist or healthcare professional is crucial for accurate diagnosis and personalized treatment options for drug-induced acne.
Methamphetamine and Alcohol Abuse: Skin Effects
Methamphetamine and alcohol abuse can both contribute to the development of acne and other skin issues. These substances can have detrimental effects on the skin, leading to various skin problems that can be both physically and emotionally distressing.
Individuals who abuse methamphetamine may experience a condition known as "meth acne," which is characterized by the formation of red, inflamed pimples. This type of acne is caused by the stimulant properties of methamphetamine, which can stimulate the oil glands in the skin and lead to excess oil production. Additionally, methamphetamine abuse can cause skin picking and scratching behaviors, which can further aggravate the skin and lead to scarring.
Alcohol abuse, on the other hand, can disrupt the normal functioning of the skin and lead to a variety of skin problems. Excessive alcohol consumption can dehydrate the skin, making it more prone to dryness, flakiness, and irritation. It can also dilate blood vessels, causing redness and flushing. Moreover, alcohol abuse can impair the liver's ability to detoxify the body, leading to a buildup of toxins that can manifest as skin issues such as acne, rashes, and inflammation.
It is important to note that methamphetamine and alcohol abuse not only affect the skin but also have serious implications for overall health and well-being. Seeking professional help to address substance abuse issues is crucial for both the physical and mental health of individuals struggling with addiction.
Drug Abuse and Skin-Related Issues
Drug abuse can have severe consequences on the skin, causing a range of issues like necrosis, fibrosis, and ulcers. When drugs are abused, they can directly impact the health and appearance of the skin, leading to various skin-related problems. These issues can manifest in different ways, including the development of necrotic skin tissue, fibrous changes within the skin, and the formation of painful ulcers.
In addition to necrosis, fibrosis, and ulcers, drug abuse can also result in the occurrence of pustulosis and vasculitis. Pustulosis refers to the formation of pustules on the skin, which are small, pus-filled bumps often accompanied by redness and inflammation. Vasculitis, on the other hand, is the inflammation of blood vessels within the skin, leading to visible red or purple discoloration, pain, and the formation of ulcers.
It is important to note that these skin issues are not limited to a specific drug or type of substance abuse. Drug abuse in general, whether it involves illicit drugs, prescription medications, or even over-the-counter substances, can have adverse effects on the skin. The severity and specific manifestations of these skin-related problems can vary depending on factors such as the type and duration of drug abuse, individual susceptibility, and overall health.
If you or someone you know is struggling with drug abuse and experiencing skin-related issues, seeking medical care is crucial. Medical professionals can provide appropriate treatment and help address both the underlying addiction and the resulting skin problems. It is also essential to quit drug use as part of the treatment process, as this can significantly improve the chances of successfully treating drug-induced acne and other related skin conditions.
Importance of Seeking Medical Care
It is crucial to seek medical attention for drug-induced acne and associated skin conditions to ensure proper treatment. When experiencing drug acne symptoms, identifying the underlying cause is essential to provide effective management. Consulting a healthcare professional or dermatologist is highly recommended.
Medical care plays a significant role in the diagnosis and treatment of drug-induced acne. A qualified healthcare provider can accurately identify the characteristics of drug acne and differentiate it from other skin conditions. This diagnosis is crucial for determining the appropriate course of action and preventing further complications.
Why is seeking medical care important?
- Accurate diagnosis: A healthcare professional can assess your symptoms, medical history, and medications to identify the specific drug causing the acne. This information is vital for effective treatment.
- Tailored treatment plan: A dermatologist can provide personalized treatment options based on the severity of your drug-induced acne, considering factors such as your skin type and any existing skincare routines.
- Prevention of complications: Seeking medical care can help prevent potential complications associated with drug-induced acne, such as secondary infections or worsening of the skin condition.
- Monitoring and follow-up: Regular visits to a healthcare professional ensure close monitoring of your progress and allow for adjustments in treatment if necessary.
In conclusion, seeking medical care for drug-induced acne and associated skin conditions is crucial for accurate diagnosis and effective treatment. With the guidance of a healthcare professional, you can take the necessary steps to manage and alleviate the symptoms, improving the overall health and appearance of your skin.
Quitting Drug Use for Treating Drug-Induced Acne
Quitting drug use is a crucial part of the treatment process for drug-induced acne and related skin issues. When drug-induced acne occurs, it is important to identify the specific drug causing the eruption and discontinue its use immediately. By eliminating the offending drug from your system, you give your skin a chance to heal and prevent further breakouts.
Along with quitting drug use, there are other steps you can take to treat drug-induced acne effectively. One option is to consult a healthcare professional who can provide guidance and prescribe appropriate treatment. Antihistamines can help alleviate pruritus, or itching, associated with the skin eruptions. Additionally, oral antibiotics may be prescribed to treat any secondary infections that may have developed as a result of drug-induced acne.
It is important to note that the timeline for improvement and resolution of drug-induced acne may vary depending on the individual and the specific drug involved. In some cases, discontinuing the drug may lead to a complete remission of symptoms within a few weeks. However, it is recommended to follow up with a healthcare professional to monitor the progress and adjust the treatment plan if necessary.
Remember, quitting drug use is not only beneficial for treating drug-induced acne but also for overall health and well-being. If you are struggling with drug abuse or addiction, seeking professional help is essential. By addressing the root cause of the problem and receiving appropriate treatment, you can improve your skin condition and embark on a path towards a healthier, drug-free life.
Conclusion
Drug acne presents with specific symptoms and characteristics that need to be identified and appropriately treated to achieve remission and maintain healthy skin. This common skin condition, also known as drug-induced acne or acneiform eruptions, occurs as a result of certain medications. The appearance of drug acne can vary, but it is typically characterized by a sudden eruption of inflammatory papules and pustules that are often itchy and located in the hair follicles. Unlike traditional acne, drug-induced acne is not preceded by visible comedones.
Systemic drugs such as corticosteroids, lithium, vitamin B12, thyroid hormones, halogen compounds, antibiotics, antituberculosis drugs, antiepileptic drugs, cyclosporin A, isotretinoin, and others can all cause drug acne. Additionally, topical products like cosmetics, especially in women, can also lead to acneiform eruptions. However, discontinuing the use of the triggering drug typically results in symptom remission.
When it comes to treatment, antihistamines can be used to alleviate pruritus (itchiness) associated with drug-induced acne, while oral antibiotics are often prescribed for secondary infections. It is important to seek medical care to accurately identify drug-induced acne and ensure appropriate treatment. It's also crucial to address any underlying drug abuse issues to prevent further skin-related problems. Methamphetamine and alcohol abuse can cause acne and other skin issues, while drug abuse in general can lead to serious conditions like necrosis, fibrosis, ulcers, pustulosis, and vasculitis.
In conclusion, recognizing the symptoms and characteristics of drug-induced acne is essential for effective treatment and achieving long-term remission. Seeking medical care, discontinuing the use of triggering drugs, and adopting a comprehensive approach to addressing any underlying drug abuse issues are crucial steps in managing drug acne and maintaining healthy skin.

FAQ
What does drug acne look like?
Drug acne is typically characterized by a sudden eruption of inflammatory papules and pustules on the skin. It is often pruritic and follicular and is not preceded by visible comedones.
What are the different types of drug acne?
There are various types of drug acne, including drug-induced acneiform eruptions. These can be caused by systemic drugs such as corticosteroids, lithium, vitamin B12, thyroid hormones, halogen compounds, antibiotics, antituberculosis drugs, antiepileptic drugs, cyclosporin A, isotretinoin, and others. Topical products such as cosmetics can also lead to acneiform eruptions, especially in women.
What are the characteristics of drug acne?
Drug acne is characterized by the sudden appearance of inflammatory papules and pustules on the skin. It is often itchy and localized to hair follicles. Visible comedones are usually not present.
How are systemic drugs related to drug acne?
Systemic drugs such as corticosteroids, lithium, vitamin B12, thyroid hormones, halogen compounds, antibiotics, antituberculosis drugs, antiepileptic drugs, cyclosporin A, isotretinoin, and others can cause drug acne. These drugs can disrupt the normal functioning of the skin and lead to the development of acneiform eruptions.
Can topical products like cosmetics cause drug acne?
Yes, topical products such as cosmetics can lead to drug-induced acneiform eruptions, especially in women. Certain ingredients in these products can irritate the skin and trigger the development of acne-like lesions.
What are the treatment options for drug-induced acne?
Treatment options for drug-induced acne include the use of antihistamines to relieve itching and oral antibiotics to treat secondary infections. It is important to consult a healthcare professional for an accurate diagnosis and appropriate treatment.
Can methamphetamine and alcohol abuse cause acne and other skin problems?
Yes, methamphetamine and alcohol abuse can contribute to the development of acne and other skin problems. These substances can disrupt the normal functioning of the skin and lead to various dermatological issues.
How does drug abuse affect the skin?
Drug abuse can cause various skin-related issues, including but not limited to necrosis, fibrosis, ulcers, pustulosis, and vasculitis. These conditions can have serious implications for overall skin health and require medical attention.
Why is seeking medical care important for drug-induced acne?
Seeking medical care is crucial for drug-induced acne because a healthcare professional can accurately diagnose the condition and recommend appropriate treatment. They can also address any underlying issues related to drug use.
Is quitting drug use necessary for treating drug-induced acne?
Yes, quitting drug use is an essential step in effectively treating drug-induced acne. Continued drug use can worsen the condition and hinder the effectiveness of other treatment measures.



































































































































